If you’re considering dental implants, one factor matters more than most people realise: your gum health. Strong, healthy gums are the foundation of long-term implant success, while untreated gum disease can lead to complications—even implant failure.In this guide, we explain the link between gum disease and dental implants, how to prepare your mouth, and why a gum health check in Hammersmith is the first step to a successful treatment.
What Are Dental Implants and Why Do Gums Matter?
A dental implant is a small titanium post placed into your jawbone to act as a replacement root for a missing tooth. Over time, it fuses with the bone in a process called osseointegration, creating a stable base for a crown.
But this process doesn’t happen in isolation—your gums play a crucial supporting role.
However, implants rely on healthy gums for protection and support. Your gum tissue:
- Forms a seal around the implant
- Prevents bacteria from entering
- Supports healing after surgery
- Maintains long-term implant stability
Without healthy gums, even the best implant treatment can fail.
Gum Disease and Dental Implants: Why It’s a Risk
One of the biggest threats to implant success is gum disease (periodontal disease).
How gum disease affects implants:
- Increases risk of peri-implantitis (infection around the implant)
- Causes bone loss, weakening implant support
- Slows healing after implant surgery
- Raises the chance of implant failure
Studies show patients with untreated periodontal disease have significantly lower implant success rates.
Signs You May Need a Gum Health Check Before Implants
Before starting implant treatment, your dentist will assess your gums carefully.
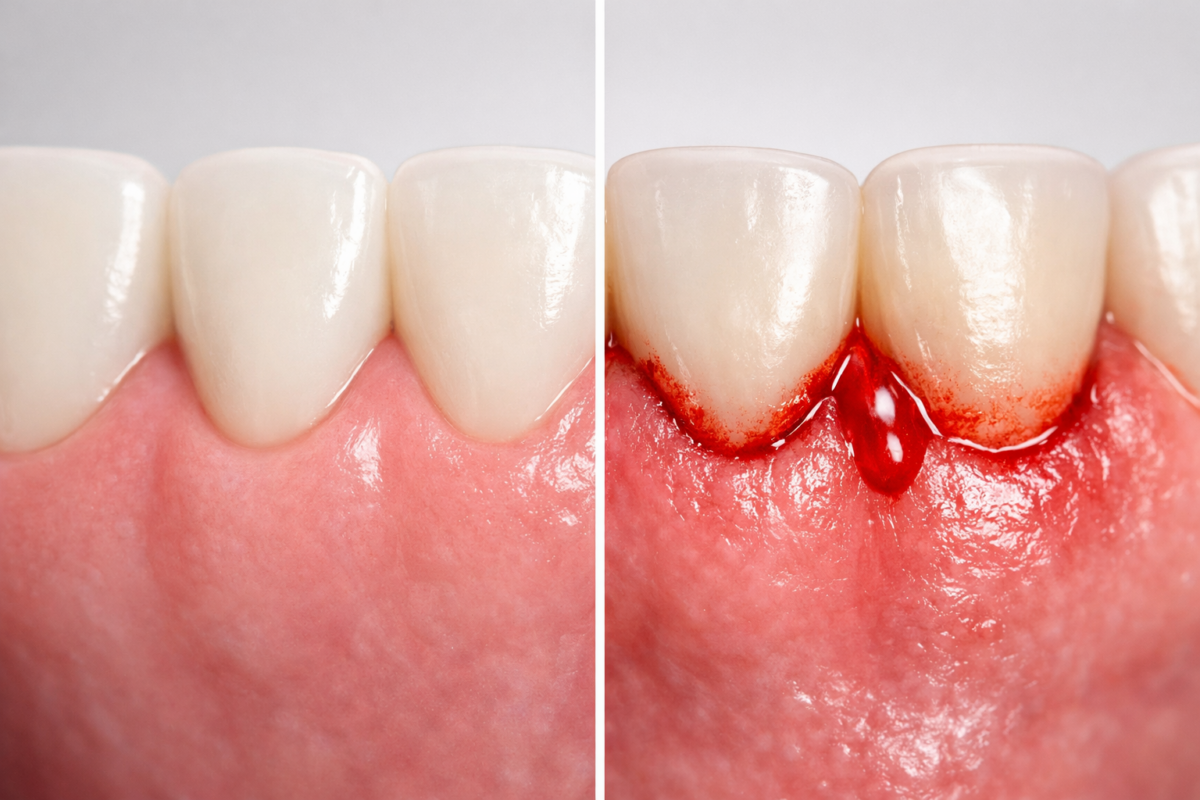
Watch for these common symptoms:
- Bleeding when brushing or flossing
- Red, swollen, or tender gums
- Gum recession (teeth look longer)
- Persistent bad breath
- Loose teeth
If you notice any of these, you may need treatment before implants.
How to Improve Gum Health Before Dental Implants
The good news is that improving your gum health can significantly increase implant success rates.
Step-by-step preparation:
- Gum Health Check (Periodontal Screening)
A full assessment identifies early signs of gum disease and bone loss.
- Professional Cleaning
Scaling and root planning remove bacteria below the gum line.
- Ongoing Hygiene Maintenance
Regular hygiene visits help keep gums healthy before and after implants.
Can You Get Dental Implants with Gum Disease?
Yes—but only after treatment.
- Gingivitis (early stage) → Reversible with professional cleaning
- Periodontitis (advanced stage) → Requires stabilisation before implants
In some cases, additional treatments such as bone grafting may be needed before implant placement.
Long-Term Implant Success Depends on Gum Care
Dental implants can last 15+ years or even a lifetime—but only with proper care.
To maintain results:
- Brush twice daily
- Clean between teeth (floss/interdental brushes)
- Attend regular hygiene appointments
- Schedule routine gum health checks
Poor gum care after implants can lead to peri-implantitis, one of the main causes of implant failure.
Dental Implants in Hammersmith: Why Gum Health Comes First
If you’re looking for dental implants in Hammersmith or West London, starting with a gum health check is essential.
At Hammersmith Dental Care, we combine:
- Preventive periodontal care
- Advanced implant dentistry
- Personalised treatment planning
This ensures your gums are in the best possible condition before implant placement—maximising long-term success.
FAQs: Gum Disease and Dental Implants
Can gum disease cause dental implant failure?
Yes. Untreated gum disease is a leading cause of implant failure due to infection and bone loss.
How do I know if my gums are healthy enough for implants?
A professional gum health check (periodontal screening) is the only reliable way to assess readiness.
How long should gums heal before implants?
This depends on the severity of gum disease, but typically ranges from a few weeks to several months after treatment.
Conclusion: Healthy Gums = Successful Implants
Your gums are the foundation of your dental implant treatment.
By addressing gum disease early and maintaining good oral hygiene, you can dramatically improve your chances of long-term implant success.
Book Your Gum Health Check in Hammersmith
Thinking about dental implants? Start with your gums.
Book your gum health check in Hammersmith today at Hammersmith Dental Care and take the first step toward a healthy, confident smile.